- Abnormal positions of the lashes and malposition of the eyelid margin often coexist: inflammatory, infectious, autoimmune or iatrogenic reasons cause inflammatory processes in the eyelid edge and in the hair bulbs contained in it. The post inflammatory healing can induce changes in the normal anatomical eyelid structure resulting the malposition of the eyelashes.
- The local medical treatment of malposition of eyelashes has only the purpose of reducing the irritative symptoms.
- Surgical procedures vary depending on the extension of malpositions and fall into two categories: ‘destruction’ and/or ‘repositioning’ of eyelashes/hair follicles.
DEFINITION.
In the upper eyelid there are approximately 100 lashes while in the lower one 50. The eyelashes originate from the anterior portion of the lid margin, in front of the tarsal plate (anterior layer), and are on two or three rows. We can find some eyelashes at the level of the caruncle. From the embryological point of view eyelashes and the Meibomian glands differentiate during the second month of gestation, starting from the same germ epithelial cells (1).
Trichiasis: altered orientation of lashes that, even if they emerge physiologically at the level of the anterior layer, are in contact with the ocular surface. Eyelashes with abnormal direction can affect the total upper and/or lower eyelid, or a portion thereof.
Distichiasis: presence of a double row of eyelashes, the first one resulting from the anterior layer while the other one, metaplastic, from the posterior layer (orifices of the Meibomian glands).
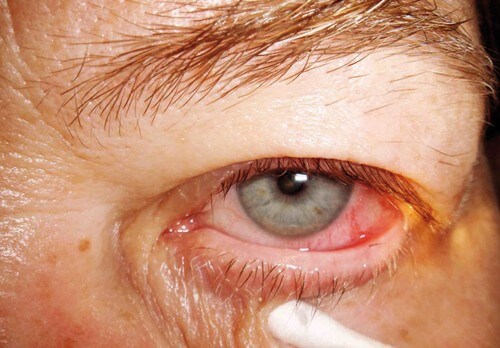
Aberrant lashes: metaplastic lashes that originate from the orifices of the Meibomian glands, located in the back layer (Pictures 1).



PICTURES 1-4: by Dr. Carlo Graziani
All malpositions of the eyelashes can cause eye irritation, epiphora, abrasion and / or corneal ulcers with loss of corneal transparency and more or less serious reduction of vision
CLASSIFICATION.
The malposition of the eyelid margin and abnormal positions of the eyelashes often coexist: inflammatory causes (chronic blepharitis, Stevens-Johnson Syndrome; vernal keratoconjunctivitis), infectious reasons (trachoma: Picture 2; herpes zoster; parasitosis: dermodex folliculorum), autoimmune causes (ocular pemphigoid scar), or iatrogenic causes (resulting from surgeries: lower blepharoplasty, correction of fracture of the orbital floor, enucleation, ectropion correction; they are secondary to trauma by chemical or physical agents) (3) lead to inflammatory processes in the eyelid edge and the bulbs hair contained therein. The post inflammatory healing can induce changes in the normal anatomical structure of eyelid with consequent malposition of the eyelashes (trichiasis).
Distichiasis can be acquired or congenital (1). The acquired form is secondary to inflammatory, infectious, autoimmune or traumatic processes involving the eyelid margin.
The congenital form can be inherited with an autosomal dominant mechanism, but it can also be associated with ptosis, strabismus, congenital heart defects, mandibulofacial dysostosis or congenital lymphoedema (4). It may remain asymptomatic until the age of 4-6 years, when direct eyelashes against the eye surface become stronger, increasing their abrasive action.
The ìetiopathogenesis of aberrant eyelashes is related to the lack of differentiation in the Meibomian gland of epithelial germ cells, that become pilosebaceous units.
MEDICAL THERAPY.
The local medical treatment of malposition of the eyelashes, with lubricants in drops, with creams or through the application of therapeutic contact lens, has the only purpose of reducing the irritative symptoms, resulting from the rubbing of the eyelashes against the eye surface.
SURGICAL THERAPY.
Numerous surgical procedures have been described for the treatment of malposition of the eyelashes (5). Different techniques are used depending on the extent of such malpositions (Table 1) (6-13). The various procedures related to the two categories ‘destruction’ and/or ‘repositioning’ of eyelashes/follicles, can be used separately or in combination. The ‘repositioning’ techniques, generally used for the entropion correction can sometimes be useful in the treatment of malposition of the eyelashes because the malposition of the eyelid margin and trichiasis often coexist (table 2), while the ‘destruction’ techniques of eyelashes and follicles are used in a specific way for the treatment of malposition of the eyelashes.
IATROGENIC COMPLICATIONS.
Possible intra- and post-operative complications, that should be discussed with the patient, are: bleeding, infection, recurrence, re-intervention, scars and alteration of the normal palpebral profile.
All eyelid malposition, if untreated, can lead to abrasions, corneal leucomas, keratitis and blindness
BIBLIOGRAPHY.
- Scheie HG, Albert DM. Distichiasis and trichiasis: origin and management. Am J Ophthalmol. 1966;61:718-20.
- West ES, Munoz B, Imeru A. The association between epilation and corneal opacity among eyes with trachomatous trichiasis. Br J Ophthalmol. 2006;90:171-4.
- Collin RJO. Entropion and trichiasis. In: A Manual of Systemic Eyelid Surgery. New York: Churchill-Livingstone;1989: 7-26.
- Samlaska CP. Congenital lymphedema and distichiasis. Pediatr Dermatol. 2002 Mar-Apr;19(2):139-41
- Bartley GB, Bullock JD, Olsen TG, Lutz PD. An experimental study to compare methods of eyelash ablation. Ophthalmology. 1987;94:1286-9.
- Johnson RL, Collin JR. Treatment of trichiasis with a lid cryoprobe. Br J Ophthalmol. 1985;69:267-70.
- Wojono TH. Lid splitting with lash resection for cicatricial entropion. Ophthalmic Plast Reconst Surg. 1992;8:287-289.
- Wood JR, Anderson RL. Complications of cryosurgery. Arch Ophthalmol. 1981;99:460-3
- West ES, Alemayehu W, Munoz B. Surgery for Trichiasis, Antibiotics to prevent Recurrence (STAR) Clinical Trial methodology. Ophthalmic Epidemiol. 2005;12:279-86.
- Tirakunwichcha S, Tinnangwattana U, Hiranwiwatkul P. Folliculectomy: management in segmental trichiasis and distichiasis. J Med Assoc Thai. 2006;89:90-3.
- Kersten RC, Kleiner FP, Kulwin DR. Tarsotomy for the treatment of cicatricial entropion with trichiasis. Arch Ophthalmol. 1992;110:714-7.
- Jordan DR, Zafar A, Brownstein S. Cicatricial conjunctival inflammation with trichiasis as the presenting feature of Wegener granulomatosis. Ophthal Plast Reconstr Surg. Jan-2006;22:69-71.
- Elder MJ, Collin R. Anterior lamellar repositioning and grey line split for upper lid entropion in ocular cicatricial pemphigoid. Eye. 1996;10:439-42.